Hearing your baby is “measuring small” is terrifying, but the key to navigating this anxiety isn’t a single percentile number—it’s understanding the growth trajectory.
- A steady growth curve, even at a lower percentile (like the 15th), is a strong sign of a healthy, “constitutionally small” baby.
- Many initial “concerning” measurements (like fundal height) are screening tools with high false-positive rates; the trend shown in follow-up ultrasounds is what matters.
Recommendation: Focus on supporting placental health through evidence-based nutrition and lifestyle choices, and work with your care team to track the growth velocity over time.
There are few phrases more terrifying for expectant parents than “your baby is measuring small.” In an instant, joy and anticipation can be replaced by a storm of anxiety. Your mind races to the worst-case scenarios, fueled by searches for terms like Intrauterine Growth Restriction (IUGR). As an ultrasound technician, I see this fear in parents’ eyes every day. The conventional advice is often a simple “don’t panic,” but that’s easier said than done when you’re faced with a number on a chart that seems to spell trouble.
Many well-meaning guides will tell you to eat more or that percentiles are just a guide. While true, this advice often misses the most crucial point. The panic comes from a feeling of powerlessness and a lack of understanding of what the data actually represents. Is it an isolated blip? A sign of a real problem? What is the difference between a baby who is simply small and a baby who is not growing properly? The key to managing this anxiety isn’t to ignore the numbers, but to understand them on a deeper level.
The truth is that the most important metric isn’t a single percentile; it’s the growth velocity, or the baby’s own personal growth curve over time. This guide will take you inside the monitoring process. We will decode the measurements, separate the “signal” from the “noise,” and empower you to see the full picture. By understanding the ‘why’ behind the ‘what,’ you can shift from being a worried bystander to an informed, confident partner in your baby’s prenatal care.
This article will walk you through the key aspects of fetal growth tracking, from understanding growth spurts and measurement techniques to differentiating between a healthy, small baby and a true growth concern. Let’s explore how to read the data with confidence.
Summary: A Technical Guide to Fetal Growth Tracking
- Why Fetal Weight Gain Accelerates in Weeks 28-32?
- How to Understand Fundal Height Measurements When You Are Plus Size?
- Growth Scan or Wait-and-See: When Is Intervention Truly Warranted?
- The Diet Mistake That Doesn’t Actually Increase Fetal Size
- How to Improve Blood Flow to the Placenta Through Sleep Position?
- Why the Nuchal Translucency Scan Is Crucial at 12 Weeks even for Young Moms?
- Why Being in the 15th Percentile Is Normal if the Curve Is Steady?
- Fetal Brain Development: Does Playing Classical Music Actually Boost Your Baby’s IQ?
Why Fetal Weight Gain Accelerates in Weeks 28-32?
The third trimester is often called the “homestretch,” and for a good reason: it’s when your baby’s growth shifts into high gear. While development has been happening steadily since conception, the period between 28 and 32 weeks marks a significant acceleration in weight gain. During this time, the primary focus of development shifts from forming organ systems to laying down fat stores and rapidly increasing in size. This is a crucial phase for building the reserves your baby will need for life outside the womb.
Think of the first two trimesters as building the factory and the third as running production at full capacity. The skeletal structure is in place, the major organs are functional, and now the baby’s job is to bulk up. This rapid weight gain is powered by the placenta, which is working at peak efficiency to transfer nutrients and oxygen. It’s not uncommon for a fetus to gain around half a pound per week during this window. This acceleration is a completely normal and vital part of pregnancy.
Understanding this biological process is the first step in contextualizing growth measurements. If a scan at 27 weeks showed your baby on the smaller side, a follow-up at 31 weeks might show a significant jump in percentile. This isn’t necessarily a sign of a previous error; it’s often just a reflection of this natural growth spurt. The body is programmed for this rapid accumulation of weight, preparing the baby for birth and the transition to newborn life. It’s a period of dramatic, visible change that we track closely on ultrasound.
How to Understand Fundal Height Measurements When You Are Plus Size?
One of the most common, and most anxiety-inducing, screening tools for fetal growth is the fundal height measurement. This is when your doctor or midwife uses a simple measuring tape to measure the distance from your pubic bone to the top of your uterus. It’s a quick, non-invasive way to get a rough estimate of fetal growth. However, it’s critical to understand that this is a screening tool, not a diagnostic one, and its accuracy can be influenced by many factors, particularly maternal body composition.
For plus-size mothers, the fundal height measurement can be especially tricky. The layer of subcutaneous adipose tissue on the abdomen can make it difficult to accurately palpate the top of the uterus, potentially leading to measurements that are larger or smaller than expected. In fact, medical research confirms that having a BMI of 30 or more can significantly affect the accuracy of this measurement. This is a perfect example of “measurement noise”—data that can be misleading without proper context.
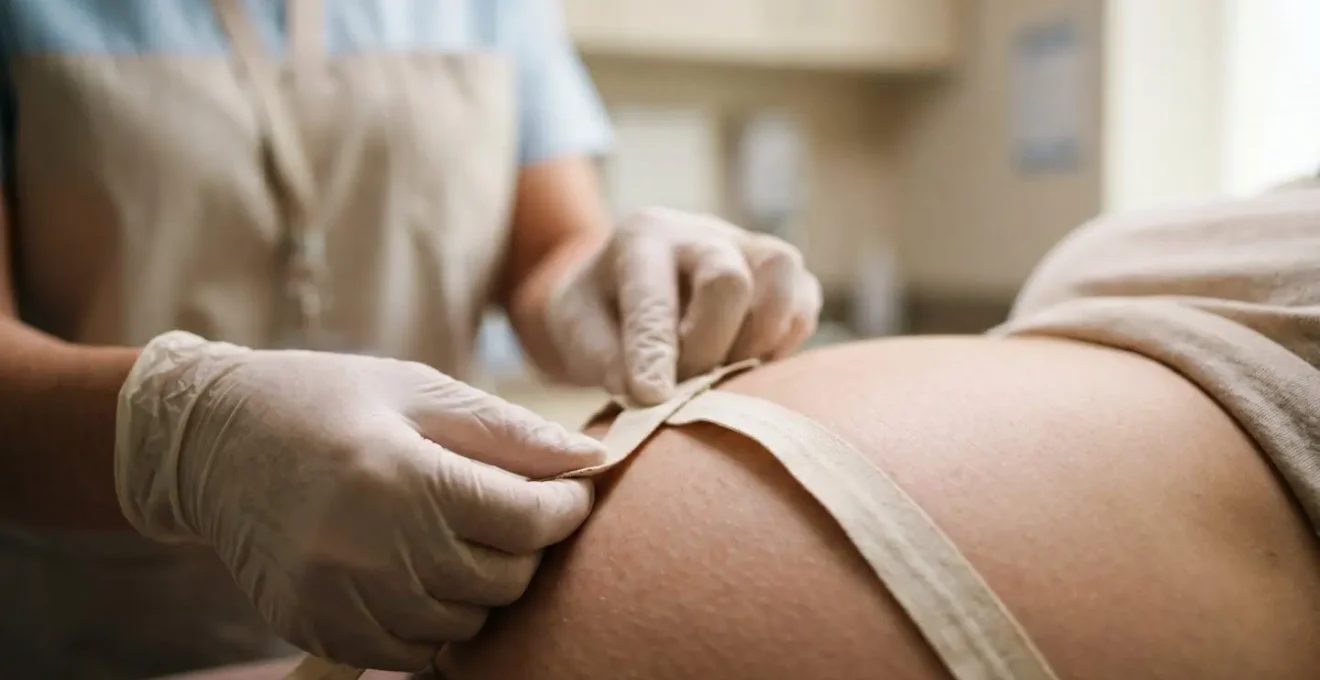
As the image above illustrates, the technique relies on manual palpation and positioning. A different provider, the baby’s position (e.g., transverse lie), or the amount of amniotic fluid can all alter the number on a given day. If your fundal height is measuring “off,” it is not an automatic cause for alarm. For plus-size moms, it is very often the trigger for a growth ultrasound, which will provide a much more precise and reliable assessment of the baby’s size. Think of the fundal height as a simple flag; it tells us to look closer, but it doesn’t define the situation.
Growth Scan or Wait-and-See: When Is Intervention Truly Warranted?
So, a fundal height measurement or a routine scan has flagged your baby as “small.” The next step is usually a detailed growth scan. This is where we, as technicians, take precise biometric measurements of the baby’s head, abdomen, and femur to calculate an Estimated Fetal Weight (EFW). This EFW is then plotted on a growth chart to determine its percentile. The crucial question then becomes: what does this number mean? Is it time to intervene, or is it a “wait-and-see” situation?
The answer lies in differentiating between a baby that is Small for Gestational Age (SGA) and one experiencing Intrauterine Growth Restriction (IUGR). An SGA baby is like a genetically small adult—perfectly healthy, just smaller than average. A significant portion of babies in lower percentiles fall into this category. In fact, medical evidence shows that of all fetuses at or below the 10th percentile, a full 40% are constitutionally small and healthy. IUGR, on the other hand, is a pathological condition where the baby is not reaching its genetic growth potential due to an underlying issue.
The Children’s Hospital of Philadelphia provides a clear clinical distinction, which is vital for parents to understand. As their team explains, the problem in IUGR is about nutrient and oxygen delivery:
IUGR occurs when the fetus does not receive the necessary nutrients and oxygen needed for proper growth and development of organs and tissues.
– Children’s Hospital of Philadelphia Medical Team, Small for Gestational Age Clinical Guide
Intervention is warranted not based on a single small measurement, but on the growth trajectory. If follow-up scans show the baby is dropping percentiles (e.g., going from the 20th to the 9th), it suggests the growth rate is slowing, and we need to investigate for IUGR with tools like Doppler ultrasounds to check blood flow. But if the baby is consistently tracking along the 15th percentile, it’s a strong indicator of a healthy, constitutionally small baby. Even in cases of true SGA, the long-term outlook is excellent, with most babies catching up in growth after birth.
Your Action Plan Before the Next Growth Scan
- Review Past Scans: Ask for the percentile from your previous scans. Your goal is to establish a personal growth curve, not just a single data point.
- List Your Questions: Write down specific questions for the doctor, such as “Is the baby following a consistent curve?” and “What do the Doppler flow measurements show?”
- Assess Your Own History: Were you or your partner small at birth? Is there a family history of smaller babies? This is crucial “constitutionally small” context.
- Track Fetal Movement: Keep a general sense of your baby’s movement patterns. A significant decrease should always be reported to your provider, as it’s a key indicator of well-being.
- Prepare for a Dialogue: Go into the appointment ready to be a partner in the monitoring process. Your goal is to understand the data, not just receive it.
The Diet Mistake That Doesn’t Actually Increase Fetal Size
When told their baby is measuring small, many parents’ first instinct is to drastically increase their food intake. The logic seems simple: “If I eat more, the baby will get more and grow bigger.” This often leads to loading up on calories, particularly from simple carbohydrates and sugary foods, in a desperate attempt to move the needle on the growth chart. Unfortunately, this is a common and largely ineffective strategy. Unless a mother is severely malnourished, simply “eating for two” in terms of calories does not directly translate to increased fetal weight.
The limiting factor in fetal growth is rarely the *quantity* of calories the mother consumes, but rather the *efficiency* of the placenta in transferring nutrients. The placenta is the gateway, and if it’s not functioning optimally, no amount of extra maternal calories will solve the problem. In fact, a diet high in processed foods and sugar can increase inflammation and may even negatively impact placental function. The focus shouldn’t be on sheer volume but on nutrient density.
Instead of just eating *more*, the key is to eat *smarter*. A diet rich in protein, healthy fats, and micronutrients supports both your health and placental function. One particularly important but often overlooked nutrient is choline. Choline is vital for fetal brain development and placental health. Rather than overeating, ensuring you are meeting specific nutritional targets is a far more effective strategy. For example, the American College of Obstetricians and Gynecologists recommends 450 mg of choline each day during pregnancy. Foods like eggs, lean meat, and legumes are excellent sources. This targeted approach supports the underlying systems of growth, which is more effective than simply trying to “fatten up” the baby.
How to Improve Blood Flow to the Placenta Through Sleep Position?
Continuing with the theme of supporting the system rather than force-feeding it, one of the most practical and evidence-based ways you can support placental function is through your sleep position. The goal is to maximize blood flow to the uterus and placenta, ensuring a steady supply of oxygen and nutrients for your baby. This is all about simple physics and anatomy. Your largest vein, the inferior vena cava, runs along the right side of your spine. When you lie flat on your back, the weight of your growing uterus can compress this vein, potentially reducing blood return to your heart and, consequently, blood flow to the placenta.
For this reason, healthcare providers universally recommend sleeping on your left side. This position takes the weight of the uterus off the inferior vena cava, allowing for optimal blood circulation. While sleeping on your right side is still better than your back, the left side is considered the gold standard for maximizing placental perfusion. It’s a small, simple adjustment that can have a meaningful impact on the efficiency of your baby’s life-support system.

Making this position comfortable is key to sticking with it. As shown in the image, using pillows is your best strategy. Placing a pillow between your knees helps align your hips and reduce back strain. Another pillow under your belly can provide support and relieve the pulling sensation. Some people even find a pillow behind their back helps prevent them from rolling over in their sleep. This isn’t about being perfectly still all night; it’s about setting yourself up for success by starting the night in the optimal position and returning to it if you wake up. It’s a tangible action you can take every single night to support your baby’s growth.
Why the Nuchal Translucency Scan Is Crucial at 12 Weeks even for Young Moms?
While much of the anxiety around fetal growth happens in the third trimester, the foundation for accurate tracking is laid much earlier. The nuchal translucency (NT) scan, typically performed around 12 weeks, is well-known as a screening tool for chromosomal abnormalities like Down syndrome. However, its importance extends far beyond that, especially in the context of monitoring growth throughout the entire pregnancy. This scan provides the most accurate dating of the pregnancy, which is the bedrock of all subsequent growth assessments.
During the first trimester, all fetuses grow at a very predictable rate, with little variation due to genetics. The crown-rump length (CRL) measurement we take at the NT scan is therefore extremely precise for establishing the estimated due date (EDD). An accurate EDD is non-negotiable. If the due date is off by even a few days, a perfectly normal-sized baby could appear “small for gestational age” on a chart later in pregnancy simply because they are being compared to the wrong standard. This is why the NT scan is crucial for all mothers, regardless of age or risk factors.
This early, precise measurement establishes the baseline for your baby’s unique growth curve. All future measurements—at the 20-week anatomy scan and any later growth scans—will be plotted against this initial dating. It allows us to distinguish between a baby who is consistently small (and likely healthy) and a baby whose growth rate is faltering. Without this reliable starting point, interpreting growth patterns becomes much more difficult. Studies on fetal growth, like the comprehensive one from the NICHD, rely on this precise dating to build their models, with the National Institute of Child Health and Human Development study establishing that growth calculations are accurate from 10 weeks 0 days to 41 weeks 6 days, underscoring the importance of that early window.
Key Takeaways
- A consistent growth curve, even at a lower percentile, is the most important indicator of a healthy baby.
- Screening tools like fundal height have high error rates; follow-up ultrasounds provide the real data.
- Focus on supporting placental health with nutrient-dense foods and proper sleep positioning, not just increasing calories.
Why Being in the 15th Percentile Is Normal if the Curve Is Steady?
This is the heart of the matter. You’ve been told your baby is in the 15th percentile. Your immediate thought is, “That’s low. Is my baby okay?” The answer, in the vast majority of cases, is a resounding yes. A percentile is not a test score; it is a comparison. Being in the 15th percentile simply means that in a group of 100 babies at the same gestational age, your baby is larger than 14 of them and smaller than 85. By definition, someone has to be in the 15th percentile, just as someone has to be in the 50th or 95th.
The clinical threshold for concern, where a baby is officially designated as Small for Gestational Age (SGA), is typically set as being below the 10th percentile. This means a baby at the 15th percentile is, by definition, considered within the normal range. The key factor that determines health is not the absolute number, but the consistency of the growth trajectory. If your baby was at the 16th percentile at 20 weeks, the 15th at 28 weeks, and is still at the 15th at 32 weeks, this is not a sign of a problem. It’s a sign of a healthy baby who is consistently and reliably following their own unique, genetically predetermined growth curve. This is what we call a “constitutionally small” baby.
Furthermore, it’s crucial to remember the high false-positive rate of initial screenings that might lead to these concerns. A single “off” fundal height measurement can cause immense stress, but it’s often just measurement noise. In fact, the data on this is incredibly reassuring. As Emily Oster highlights in her analysis of large-scale studies, the predictive value of these initial flags is low. For instance, research from a large Swedish study shows that for 8 out of 10 people who get a concerning result from a fundal height screening, they will go on to have a normal-size baby. The real story is told by the trend line across multiple, high-quality ultrasound scans.
Fetal Brain Development: Does Playing Classical Music Actually Boost Your Baby’s IQ?
In the quest to do everything possible for their baby, parents often turn to popular “brain-boosting” activities, with the “Mozart effect” being one of the most enduring. The idea that playing classical music to the womb will increase a baby’s IQ is a tempting one, but it is, for the most part, a myth. While your baby can hear sounds from around 23 weeks and may be calmed by familiar music, there is no scientific evidence to suggest it provides any cognitive advantage. The anxiety to “optimize” your baby can lead you down paths that are not supported by evidence.
The real secret to supporting fetal brain development isn’t found in a playlist; it’s found on your plate and in your lifestyle. The same factors that support healthy overall growth are the ones that fuel the brain’s incredible development. This brings us back to the core principles: maximizing placental health and ensuring a steady supply of crucial nutrients. You don’t need to buy special headphones for your belly; you need to focus on the biological building blocks.
For instance, we’ve already discussed the importance of choline. The impact of this single nutrient on brain development is far more significant and evidence-based than the Mozart effect. In fact, randomized controlled trials demonstrate that higher maternal choline intake is associated with improved markers of infant cognitive function, including information processing speed and memory. This is the real “brain-boosting” work. By focusing on evidence-based strategies—like a nutrient-dense diet, proper sleep position, and managing stress—you are doing the most important things possible for your baby’s overall health and brain development. Trust the science and your body, not the myths.
By shifting your focus from a single, static percentile to the dynamic, ongoing story of your baby’s growth curve, you can navigate your pregnancy with information instead of anxiety. Work with your care team, ask questions, and trust in the power of consistent, evidence-based monitoring.